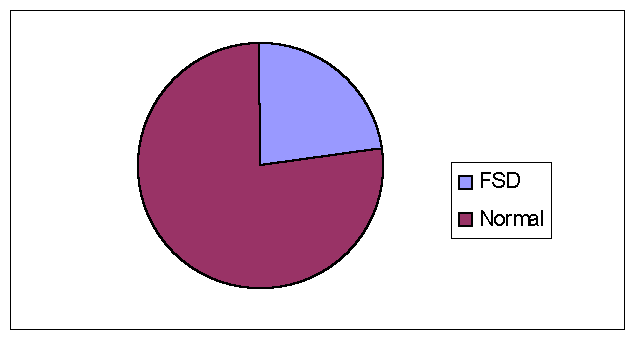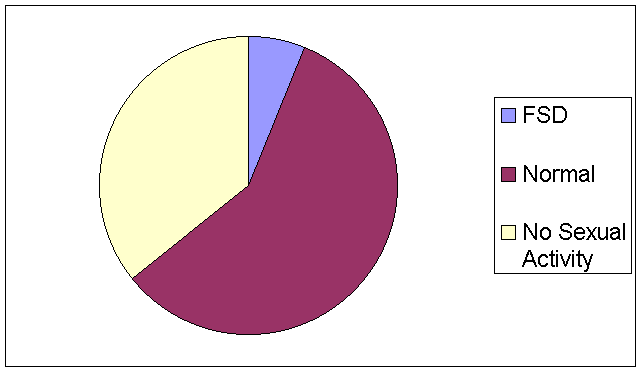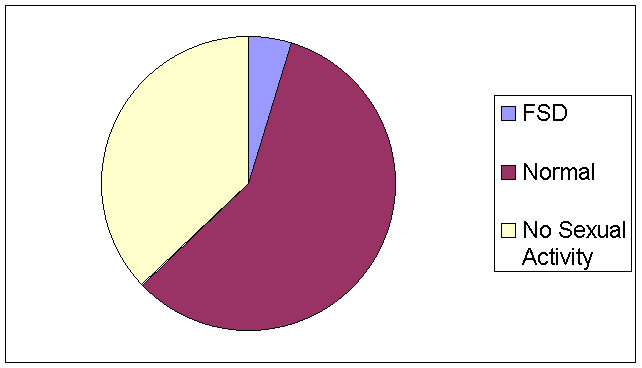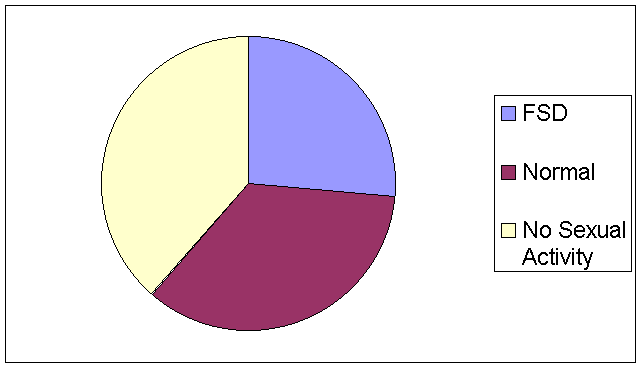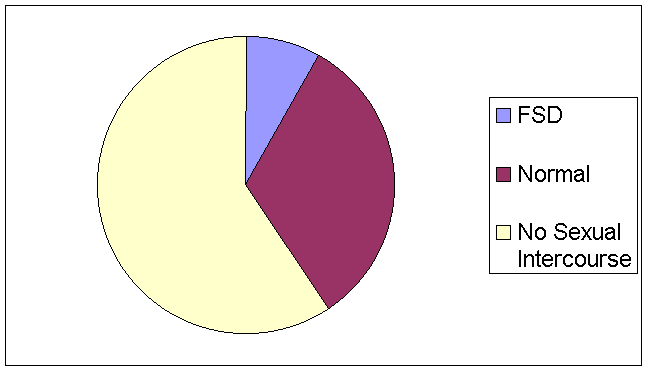Prevalence of Female Sexual Dysfunction among College Students
Jennifer Wilson
Luther College
Abstract
Female sexual dysfunction (FSD) affects about 43% of women at some point in their lifetime. The four sub-types identified by the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) are desire, arousal, orgasmic, and pain disorders related to sexual functioning. The purpose of this research was to investigate the prevalence of FSD in a college population and then to identify ways to address this issue. The results indicate that a total of 47% of the women surveyed using the Female Sexual Functioning Index have a high probability of struggling with FSD. The highest percentage of women struggle specifically with orgasmic disorder (26.4%). These high percentages call for immediate attention. Research on a college-aged population must be added to the body of research on female sexual dysfunction. Then to attempt to combat this issue, greater access to sexuality education and a heightened awareness of its impact on our society need to be addressed.
Prevalence of Female Sexual Dysfunction among College Students
Sexual dysfunctions are defined as �disorders in which people cannot respond normally in key areas of sexual functioning� (Comer, 2002, p. 309). Up to 43% of the general female population either currently struggles with, or has struggled with a form of sexual dysfunction at some time (Laumann, Paik, & Rosen, 1999; as cited in Rosen, R., Brown, C., Heiman, J., Leiblum, S., Meston, C., Shabsigh, R., Ferguson, D., & D�Agostini, R., Jr., 2000). Sexual dysfunction among women is rarely discussed and greatly overlooked. In my Abnormal Psychology course, when we discussed sexual dysfunction, it was apparent that there was a plethora of information about male sexual dysfunction, but very little on female sexual dysfunction. I was curious, so I spoke with a member of the counseling staff at my school. I was interested in what counselors did for a female student struggling with sexual dysfunction: did they have pamphlets, or other resources, or what kinds of talk therapy did they use? I was told that women on my campus do not struggle with sexual dysfunction unless there is a history of abuse. This assertion was troubling, so I decided to investigate the matter on my own. What follows is an examination of current literature on the topic of female sexual dysfunction (FSD) and a study I conducted on my college campus to determine the prevalence of FSD.
One event that sparked much attention among psychologists occurred in 2001: the International Consensus Development Conference on female sexual dysfunction (Basson, R., Berman, J., Burnett, A., Derogatis, L., Ferguson, D., Fourcroy, J., et al., 2001). The purpose of this conference was to explore the definitions and classifications of female sexual dysfunction, and deal with current assessment problems. Those at the meeting also attempted to provide identifiable endpoints for evaluation and determine the most pressing areas for future research. In many ways, the definitions that they provided are not different from those in the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV; American Psychiatric Association, 1994); in fact, the categories were purposely retained for past and future research continuity. However, a new classification category of a sexual pain disorder was created: noncoital sexual pain disorder. The definitions that were determined to be the most representative of current clinical practice and research are detailed in Table 1.
Table 1: Descriptions of the Classified Sexual Dysfunction Disorders
Disorder
Description
Sexual Desire
Hypoactive sexual desire disorder is the persistent or recurrent deficiency (or absence) of sexual fantasies/thoughts, and/or desire for or receptivity to sexual activity, which causes personal distress.
Sexual aversion disorder is the persistent or recurrent phobic aversion to and avoidance of sexual contact with a sexual partner, which causes personal distress.
Sexual Arousal
Sexual arousal disorder is the persistent or recurrent inability to attain or maintain sufficient sexual excitement, causing personal distress, which may be expressed as a lack of subjective excitement, or genital (lubrication/swelling) or other somatic responses.
Orgasmic
Orgasmic disorder is the persistent or recurrent difficulty, delay in or absence of attaining orgasm following sufficient sexual stimulation and arousal, which causes personal distress.
Sexual Pain
Dyspareunia is the recurrent or persistent genital pain associated with sexual intercourse.
Vaginismus is the recurrent or persistent involuntary spasm of the musculature of the outer third of the vagina that interferes with vaginal penetration, which causes personal distress.
Noncoital sexual pain disorder is recurrent or persistent genital pain induced by noncoital sexual stimulation.
Note. Each of these diagnoses is subtyped as A�lifelong verses acquired type, B�generalized versus situational type and C�etiologic origin (organic, psychogenic, mixed, unknown).
(Basson, et al., 2001)
This conference sparked an explosion of commentary on the conference, on its methods and/or biases, and on current research practices (Kameya, 2001; Plaut, 2001; Tiefer, 2001; Vroege, Gijs, & Hengeveld, 2001). The topic of female sexual dysfunction is very appropriate for public, professional dialogue. One common thread throughout the many commentaries was that there is simply not enough research on the subject. Most of the articles that emerged following the conference were commentaries, literary reviews and informative articles, such as Binik, Y., Reissing, E., Pukall, C., Flory, N., Payne, K., & Khalife, S. (2002) article titled, �The female sexual pain disorders: Genital pain or sexual dysfunction?� There were very few actual studies. The few studies that were conducted have explored the development and testing of new questionnaires to measure FSD (Quirk, F., Heiman, J., Rosen, R., Lann, E., Smith, M., & Boolell, M.,� 2002; Rosen et al., 2000). There were also studies that compared the psychometric properties of the available methods of self-report (Daker-White, 2002; Dennerstein, Anderson-Hunt, & Dudley, 2002).
According to the current research, FSD is beginning to be viewed as a medical problem instead of, or in addition to, a completely psychological one. Current research into the possible benefits of Viagra for women, other medications or herbs to increase arousal, and such things as vacuum therapy seem promising (Bancroft, 2002; Billups, K., Berman, L., Berman, J., Metz, M., Glennon, M., & Goldstein, I., 2001; Williams & Leiblum, 2002). Bancroft urges caution in prescribing Viagra to solve women�s sexual problems. She cites three issues to consider in the medicalization of FSD: differences between men and women in sexuality, sex therapy, and the difference between a sexual problem and a sexual dysfunction. Current research is also starting to examine the effect of certain medical problems or operations on sexual functioning (Aksaray, Yelken, Kaptonaoglu, Oflu, & �zaltin, 2001; Burchardt, M., Burchardt, T., Anatasiadis, A., Kiss, A., Baer, L., Pawar, R., de la Taille, A., Shabsigh, A., & Shabsigh, R., 2002; Hutcherson, 2002). These highlight issues such as hypertension, hysterectomies, cancer, and obsessive compulsive disorder.
Looking at sexual functioning difficulties as a purely medical problem, however, does not take into account the social and interpersonal influences on a person. Often there are greater issues that are being ignored or passed over when a pill is prescribed, for both men and women. There are other solutions to the dilemma of FSD than a medical model. Many include skills training, talk therapy, and the inclusion of the woman�s partner in therapy. There is evidence suggesting that increased education, a positive sexual upbringing, and realistic social expectations about sex lead to women who are more orgasmic (Williams & Leiblum, 2002).
An article by Heiman (2002) investigated the success of the current treatments available for FSD. She found that treatments for orgasmic disorders were the most efficacious, and treatments for pain disorders were possibly efficacious. Heiman concluded that:
�(a) since a psychologic treatment can and does impact sexual physiology, we need tocontinue to develop and test psychologic approaches both out of intellectual interest andout of respect for the choices patients require or prefer,
(b) the prescription of a physiologic treatment which ignores the fact that humansexuality is infused with individual meaning may invite further interference with sexualfunctioning, and
(c) future research would do well to test the efficacy of the psychologic and physiologictreatments, both separately and in combination, for female sexual dysfunction.�� (p. 445).As this and other articles indicate, both medical and psychological treatments for FSD need to be considered.
Many questions still remain in the field of female sexual dysfunction. One involves the question of priorities: Should the desired outcome of research be a diminished prevalence of FSD through prevention, or should research focus on finding a better treatment? There are no easy answers, and everyone has their own biases. An increased amount of both kinds of research is needed, but the short-term question remains, �What can be done right now?�
Past research indicates that sex education could be very helpful in treatment of FSD. The ideal target of sex education is one that is old enough to have had some sexual experimentation, but young enough to allow for the greatest impact of education. This population is concentrated on college campuses. Before starting a large-scale attempt at sex education and striving to make self-exploration socially acceptable for women, it would be very informative to explore the prevalence of FSD on the college campus. This population has often been overlooked; instead, current studies have focused on peri- and post-menopausal women.
The purpose of this research was to explore the prevalence of FSD at a small liberal arts college, and then use the results from this study to argue for an increased awareness of FSD and education regarding sexuality on campus. My hypothesis is that there will be fewer college-aged women struggling with FSD than in the general population, but enough to warrant further consideration of the topic.
Method
Participants
Participants were students at a private, religiously affiliated liberal arts college in the Midwest. The college strives to maintain a ratio of 60 % women to 40 % men. One hundred and fifty students ranging in age between 18 and 26 participated in this study. Two hundred and fifty women were randomly selected from among the entire female population at the college, and research was concluded after 150 surveys were administered. No one declined participation, although one woman returned the survey blank and another participant only answered two survey questions and partially filled out the demographic page.
Measure
The survey utilized in this study was the Female Sexual Function Index (FSFI), which was developed for use by Rosen et al. (2000). There are 19 items, each measured on a 5-point Likert scale, and most questions also have a response box for �no sexual activity.� Rosen et al. used factor analysis to determine six sub-domains measured by the FSFI, including desire, arousal, lubrication, orgasm, satisfaction, and pain. The discriminant validity, the ability of the scale to differentiate between clinical and nonclinical populations, was assessed by comparing the means of patients clinically diagnosed with FSAD (female sexual arousal disorder, n=128) with the means of normally functioning controls (n=131). There were statistically significant differences measured for each of the six sub-domains. The questionnaire has a high level of internal consistency (Cronbach�s α = .81-.97) and is also highly reliable (test-retest of .61 < r < .92) (Daker-White, 2002).
A brief demographic page was developed and administered in addition to the questionnaire. Information requested on the demographic page included age, the number of different sexual partners (for any sexual activities, as operationally defined at the beginning of the FSFI, and also specifically for sexual intercourse), whether or not the participants masturbate or have a history of abuse, and the medications the participants were currently taking. These data were used in conjunction with the results from the survey to answer some basic questions about trends in sexual functioning.
Design and Procedure
Students were approached in their dorm or phoned ahead and invited to stop by the psychology department office to fill out the questionnaire. The purpose of the study was briefly explained, both verbally and in the written consent form. Participants were informed that involvement was voluntary and that they could turn in a blank survey if they decided not to complete it. They were then asked to fill out the questionnaire and demographic page, being as honest as possible. To preserve anonymity, participants placed completed (or blank) forms in an envelope along with other forms previously collected. A debriefing handout with information pertaining to female sexual dysfunction and references to counseling, websites, and books were provided at completion of the survey.
No cut-off numbers were provided with the FSFI, only the normative data were available. The mean scores of the clinical and nonclinical populations were used as a guide to determine cut-off values for the sub-domains, as well as the scoring guide provided with another very similar questionnaire (Quirk et al., 2002). The questionnaire by Quirk et al. had slightly different questions to measure the same sub-domains. Quirk et al. were contacted with a request to use their questionnaire, but they did not respond to the request. When a discrepancy existed between the means of the FSFI and the cut-off scores of the other questionnaire, the more conservative number was used. This was the case in all sub-domains except the pain category, where it was more meaningful to use a slightly less conservative cut-off score of 10, keeping in mind that the average score of the clinical population was even higher than 10. Scores of the following magnitudes and lower were considered to have a high probability of having sexual functioning difficulties: Desire: 4, Arousal: 10, Lubrication: 10, Orgasm: 8, Satisfaction: 8, Pain: 10.
Results
The total percent of women with at least one of the measured difficulties in sexual functioning was 47% when the sub-domain of satisfaction was not included. Including the sub-domain of satisfaction (which is not a specific sexual dysfunction as recognized by the DSM-IV, but is an important criteria for receiving a diagnosis of dysfunction), the percentage climbs to 67.8% of the surveyed women.
The percentage of women who have engaged in some form of sexual activity and who are struggling with some form of sexual dysfunction is 41.3%. The questionnaire provides the opportunity to indicate that no sexual activity has occurred for questions regarding arousal, lubrication, orgasmic and pain disorders.� It is important not to discount the validity of a desire disorder; however, participants could answer the desire questions whether they had engaged in any sexual activity or not.
As indicated by the response to the question on the demographic page regarding abuse, 90% of those struggling with some form of FSD (again not including the sub-domain of satisfaction) had no history of abuse. As measured by the FSFI, 58% of the women in this study with a history of abuse were likely to have at least one form of FSD as measured by the DSM-IV.
For the category of desire, 22.8% of the surveyed population reported sexual functioning difficulties as defined by our cut-off scores (see Figure 1). That is, 34 of the 149 valid surveys indicated problems in the desire domain of sexual functioning.
Figure 1. Percent of women with desire functioning difficulties
Figure 2 shows the results of the arousal category, where only 6.1% of the 148 who answered the question reported arousal problems. Thirty-six percent of the surveyed population reported no relevant sexual activity, and 58.1% reported normal functioning. Thus, for those reporting some sexual activity, actually 9.5% have a high probability of having a sexual arousal disorder.
Figure 2. Percent of women with arousal functioning difficulties
A similar trend was noticeable in the lubrication category: 4.7% of those surveyed reported lubrication difficulties. Again, 37.2% of the population reported having no sexual activity in the past 4 weeks, and 58.1% reported normal functioning (see Figure 3). Here, the percent of sexually active participants with lubrication difficulties jumps to 7.5%.
Figure 3. Percent of women with lubrication functioning difficulties
A much larger 26.4% of the surveyed population expressed orgasm problems as shown in Figure 4; again, 38.5% reported no sexual activity, and only 35.1% had a high probability of functioning normally. When only those who have engaged in sexual activity in the past 4 weeks are accounted for, actually 42.9% of sexually active women may have had an orgasmic disorder.�As Figure 5 depicts, a high 42.6% claimed dissatisfaction, and 54.7% reported being satisfied with the level and amount of sexual activity experienced.
Figure 4. Percent of women with orgasm functioning difficulties
Figure 5. Percent of women who are unsatisfied
Of the women surveyed, 8.1% reported pain difficulties with intercourse. Figure 6 shows that 59.5% of the women surveyed had not attempted intercourse in the past 4 weeks, and the remaining 32.4% claimed normal functioning. So, actually, 20% of those engaging in sexual intercourse in the previous 4 weeks have a high probability of having a sexual pain disorder.
Figure 6. Percent of women with sexual pain
Discussion
The results reveal that the percentage of college-aged women struggling with FSD is very similar to the widely cited 43% of the general female population (Laumann, Paik, & Rosen, 1999; as cited in Rosen et al., 2000). Similar liberal arts colleges may have similar percentages of women struggling with sexual functioning problems. Although the specific demographics may be different at this college than at a state school, it is a high percentage of women regardless of the unique composition of the school. Thus, one could tentatively conclude that the percentage of college-aged women struggling with FSD is very similar to the general female population.
The results for orgasmic difficulties represent a higher percentage than for any of the other categories relating specifically to sexual activity in the past four weeks, (percent for the satisfaction domain were higher, but that includes more than the past four weeks).Another troubling finding is that 20% of women who attempted sexual intercourse in the previous four weeks experienced a high degree of pain, which suggests that they may have been struggling with a sexual pain disorder.
The questions regarding satisfaction were applicable even to those who have never engaged in any sexual activity, because women were able to comment on their satisfaction with the amount of sexual activity they personally experienced. Also, in this category, 2 women answered these questions incorrectly, failing to answer the question with regards to their level of satisfaction, instead hand writing �no sexual activity�. These considerations should cause one to use caution when generalizing the results of the satisfaction category.
The results indicate that a history of abuse is not a necessary qualification to have sexual functioning difficulties, nor does it make sexual functioning difficulties more likely. When this research was initially proposed, it was suggested that the only reason women of a college age would have any sexual functioning difficulties is due to a past history of abuse. The validity of that claim is not supported by the results of this study.
Referring back to Williams and Leiblum (2002), it is interesting to note that the treatments they suggest are very simple. Sex education and permission to explore one�s body and one�s sexuality seem to be superfluous or unnecessary, yet the prevalence of FSD in society indicates that these steps are necessary.
One easy way to get started would be to form some supportive women�s groups as a forum to discuss sexuality. These small groups could be a good setting to discuss permission to explore one�s body as well as directed masturbation training. A forum could be held, or a lecture on general or specific sex education could take place.
Another good place to start would be in counseling centers on campus. Perhaps some up-to-date training in the treatment of FSD or sex education would be appropriate. Counseling centers might create an informative pamphlet on FSD, including the importance of a greater self-awareness.
The co-morbidity among the subtypes of FSD leads me to believe that addressing issues central to one specific subtype will have an effect on other subtypes as well. Treatments have been shown to be efficacious for orgasmic disorder and for pain disorders and since arousal is strongly linked to previous pain or orgasmic experience (Heiman, 2002), using treatments known to be efficacious for one subtype of FSD may have an indirect effect on other subtypes.
In future research it would be incredibly useful to investigate any correlation between the taking of birth control pills and sexual dysfunction. Two possible arguments could be made: one suggests that without the threat of pregnancy, women would have a lower prevalence of FSD. The opposing view takes into account the effect many birth control pills have on ease of lubrication and arousal functioning; the hypothesis being that the rate of FSD would be higher in those taking birth control pills. The correlation between masturbation and FSD would be interesting to investigate as well. One of the suggested treatments for FSD is directed masturbation training and permission to explore one�s body. Thus, if one regularly masturbates, the likelihood of sexual functioning difficulties should arguably be lower.
One might be concerned that a heightened awareness of FSD on campus and greater access to healthy sex education would lead to a �sex crazed� campus. In a meta-analysis by Grunseit, Kippax, Aggleton, Baldo and Slutkin (1997), 53.2% of studies showed no effect of HIV/AIDS and sexual health education on promiscuity, while 36.2% of them actually decreased age of onset of sexual activity, reduced the number of sexual partners, or reduced unplanned pregnancy. Only 6.4% of the articles showed an increase in sexual behavior due to sexual education; although, it is arguable that it might have been healthier and safer sexual activity. Other articles show very similar results of education, including the ineffectiveness of abstinence-only education (Sather & Zinn, 2002; Starkman & Rajani, 2002). Education is an empowering step aimed at giving women permission to have control over their bodies. It is not enough to say that the environment at a college does not openly endorse traditional gender roles; the campus needs to step up and actively dispute the traditional societal messages and pressures.
The purpose of this research was two-fold: to investigate the prevalence of FSD on a college campus and to investigate possible solutions to the problem if it was found. It is now evident that perceptions can be misleading and have caused us to ignore a major issue: many college-aged women do struggle with sexual functioning difficulties, and past abuse has little to do with that. As this research demonstrates, there is much that is not understood about FSD, and there is a large gap between the amount and quality of research on FSD and that on Male Sexual Dysfunction. I would like to issue a challenge to my fellow researchers: continue to stretch the boundaries of what is known about FSD, and continue to raise awareness about this important issue.
References
Aksaray, G., Yelken, B., Kaptanoglu, C., Oflu, S., & �zaltin, M. (2001). Sexuality in Women with obsessive compulsive disorder. Journal of Sex & Marital Therapy, 27, 273-277.
American Psychiatric Association. (1994). Diagnostic and statistical manual of mental disorders. (4th) ed.). Washington, DC: Author.
Bancroft, J. (2002). The medicalization of female sexual dysfunction: The need for caution.Archives of Sexual Behavior, 31, 451-455.
Basson, R., Berman, J., Burnett, A., Derogatis, L., Ferguson, D., Fourcroy, J., Goldstein, I., Graziottin, A., Heiman, J. Laan, F., Leiblum, S. Padma-Nathan, H., Rosen, R., Segraves, K., Segraves, R. T., Shabsigh, R., Sipski, M., Wagner, G., & Whipple, B. (2001).
Report of the International Consensus Development Conference on female sexual dysfunction: Definitions and classifications. Journal of Sex & Marital Therapy, 27, 83-94.
Billups, K., Berman, L., Berman, J., Metz, M., Glennon, M., & Goldstein, I. (2001). A new non-pharmacological vacuum therapy for female sexual dysfunction. Journal of Sex & Marital Therapy, 27, 435-441.
Binik, Y., Reissing, E., Pukall, C., Flory, N., Payne, K., & Khalif�, S. (2002). The female sexual pain disorders: Genital pain or sexual dysfunction? Archives of Sexual Behavior, 31, 425-429.
Burchardt, M., Burchardt, T., Anastasiadis, A., Kiss, A., Baer, L., Pawar, R., de la Taille, A., Shabsigh, A., & Shabsigh, R.. (2002). Sexual dysfunction is common and overlooked in female patients with hypertension. Journal of Sex & Marital Therapy, 28, 17-26.
Comer, R.J. (2002). Fundamentals of Abnormal Psychology (3rd ed.). New York: Worth Publishers.
Daker-White, G. (2002). Reliable and valid self-report outcome measures in sexual (dys)function: A systematic review. Archives of Sexual Behavior, 31, 197-209.
Dennerstein, L., Anderson-Hunt, M., & Dudley, E., (2002). Evaluation of a short scale to assess female sexual functioning. Journal of Sex & Marital Therapy, 28, 389-397.
Grunseit, A., Kippax, S., Aggleton, P., Baldo, M., & Slutkin, G. (1997). Sexuality education and young people's sexual behavior: A review of studies.Journal of Adolescent Research, 12, 421-453.
Heiman, J. (2002). Psychologic treatments for female sexual dysfunction: Are they effective and do we need them? Archives of Sexual Behavior, 31, 445-450.
Hutcherson, H. (2002). What Your Mother Never Told You About S-E-X. New York: G. P.Putnam�s Sons.
Kameya, Y. (2001). How Japanese culture affects the sexual functions of normal females.Journal of Sex and Marital Therapy, 27, 151-152.
Plaut, S. (2001). New diagnostic categories for female sexual dysfunction: Does the falling tree make a sound if no one is there to hear it? Journal of Sex and Marital Therapy, 27, 193-195.
Quirk, F., Heiman, J., Rosen, R., Lann, E., Smith, M., & Boolell, M. (2002). Development of a sexual function questionnaire for clinical trials of female sexual dysfunction. Journal of Women�s Health & Gender-Based Medicine, 11, 277-289.
Rosen, R., Brown, C., Heiman, J., Leiblum, S., Meston, C., Shabsigh, R., Ferguson, D., & D�Agostini, R., Jr. (2000). The female sexual function index (FSFI): A multidimensional Self-report instrument for the assessment of female sexual function. Journal of Sex & Marital Therapy, 26, 191-208.
Sather, L., & Zinn, K. (2002). Effects of abstinence-only education on adolescent attitudes and values concerning premarital sexual intercourse. Family Community Health, 25, 1-15.
Starkman, N., & Rajani, N. (2002). The case for comprehensive sex education. AIDS Patient Care and STDs, 16, 313-318.
Tiefer, L. (2001). The �Consensus� conference on female sexual dysfunction: Conflicts of interest and hidden agendas. Journal of Sex and Marital Therapy, 27, 227-236.
Vroege, J., Gijs, L., & Hengeveld, M. (2001). Classification of sexual dysfunctions in women. Journal of Sex and Marital Therapy, 27, 237-243.
Williams, N., & Leiblum, S. (2002). Sexual Dysfunction. In G. M. Wingood & R. J. DiClemente (Eds.), Handbook of Women�s Sexual and Reproductive Health (pp. 303-328). New York: Kluwer Academic/Plenum Publishers.
|
|
|
©2002-2021 All rights reserved by the Undergraduate Research Community. |